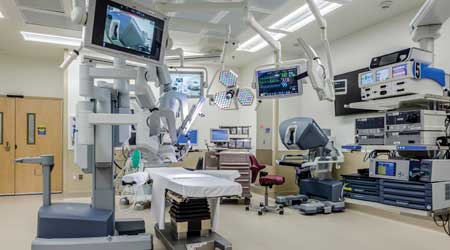
 Incorporating cable management for surgical robotics improves infection control while minimizing the disinfection process at the William P. Clements Jr. University Hospital at UT Southwestern Medical Center in Dallas, Tex. (c) CallisonRTKL
Incorporating cable management for surgical robotics improves infection control while minimizing the disinfection process at the William P. Clements Jr. University Hospital at UT Southwestern Medical Center in Dallas, Tex. (c) CallisonRTKLHow Technology is Evolving in Healthcare Facilities
From the OR to the mechanical room, new demands, practices, and yes, technology, are reshaping healthcare facilities.
Anyone with a smartphone knows that state-of-the-art technology can be outdated in 12 months or less. To accommodate change, manufacturers introduce new models, and consumers decide how often they want to replace their cell phones.
Responding to change is not that easy with healthcare facilities. There is plenty of significant change afoot, from increased competition, to new ways of delivering care, to the ever-present uncertainties of regulations and funding.
One of the biggest sources of change is advances in healthcare technology. “Technology is evolving at an incomprehensible speed,” says Tim Krawetz, senior principal at Syska Hennessy.
Those changes present a dilemma to healthcare facility managers. A hospital building, which can take five or six years from preplanning to occupancy, is bound to encounter technology refinements, or completely new technologies “may just show up,” says Krawetz.
In this environment, facility managers must ensure that their new healthcare facilities are flexible enough to accommodate new technologies, while still meeting familiar requirements for energy efficiency, code compliance, and patient/staff comfort, plus new demands for resilience.
Healthcare facility managers don’t have the luxury of building more space than they need. In a competitive healthcare market, overbuilding to accommodate future needs is not financially viable. “We don’t know exactly what the building will need during its lifespan, but we don’t want to engineer a facility that is bigger than it needs to be,” says Tariq Amlani, principal, buildings health sector Canada, for Stantec.
The solution, says Beth S. Muller, senior associate, technologies, at Jaros, Baum & Bolles, is space that is “flexible rather than overdesigned.” Medical facilities need to be rightsized for today’s functionality with areas that can be expanded or contracted with minimal disruption in the future.
A flexible grid design can allow for additional space needed for interventional radiology, robotics, imaging, or other new healthcare needs, says Dan Thomas, vice president, CallisonRTKL.
The grid enables modular design. Each element of the design fits into the modules in patterns, allowing the modules to be redone or reconfigured as healthcare needs evolve over time with minimal disruption to other areas of the building. This design modularity is one way to achieve a rightsized, flexible space without huge capital outlays and added operational costs, Amlani says.
Flexibility pays off. One teaching hospital wanted a robotics operating room (OR) that allowed for optimum flexibility to reposition the robotics for differing surgical procedures without using cabling on the floor. The solution was an infrastructure that allowed multiple simple connections with dedicated spaces for robotic equipment, a training console, and future capabilities, says Steve Juett, senior associate vice president at OneEQ, a Callison/RTKL company.
To support training, a separate observation room outside the OR with a large window to the OR was created, including multiple surgical displays that can be used to teach important elements of the surgical procedures. This strategy improved infection control by reducing student visitors to the OR. Further, the teaching OR incorporates a secondary surgeon’s console for side-by-side optimal skills training.
Striking the right balance between flexibility and rightsizing requires teamwork by all the players, especially those operating and using the healthcare facility. “We need to discover what kind of cases the stakeholders are currently seeing and what technologies they are interested in for the future,” explains Juett. “Then we go to the vendors, such as the robotics supplier, and learn what new functionalities are on the horizon.”
Related Topics:














