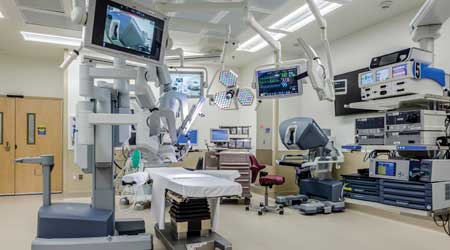
 Incorporating cable management for surgical robotics improves infection control while minimizing the disinfection process at the William P. Clements Jr. University Hospital at UT Southwestern Medical Center in Dallas, Tex. (c) CallisonRTKL
Incorporating cable management for surgical robotics improves infection control while minimizing the disinfection process at the William P. Clements Jr. University Hospital at UT Southwestern Medical Center in Dallas, Tex. (c) CallisonRTKLHow to Collaborate with IT in Healthcare Facilities
The growing importance of digital technology makes it essential for the facility manager to bring the hospital’s IT team together with the building design team.
With all the digital health practices now entering healthcare environments, says Jeff Hankin, senior principal, buildings health sector U.S. for Stantec, it’s important for healthcare facilities to have a robust infrastructure, so that systems and devices can communicate with each other from any location at any time.
All these data points are causing healthcare data centers and data rooms to have load densities that are five to 10 times higher than in the recent past, says Hankin. As information storage is growing exponentially, one strategy is to move nonessential loads outside the hospital whenever possible.

(As hospitals come to rely on digital technologies, the power system becomes even more critical than it has always been. Photo: Ari Burling/Syska Hennessy.)
Given the growing importance of digital technology, it’s essential for the facility manager to bring the hospital’s IT team together with the building design team to establish a basis of design. “Once we have an understanding of the fundamental requirements of the information technology platform, the current IT loads will be allocated in the base design, with the cabling, IT infrastructure, and support systems engineered to allow for flexible and scalable growth,” says Christopher J. Prochner, partner at Jaros, Baum & Bolles.
Both new technologies and evolving existing technologies such as passive optical networks, power over Ethernet lighting, cloud-based platforms, software-defined LAN systems, and interoperable RFID devices enable smart solutions that are efficient from the power, cooling, and space utilization perspectives, according to Prochner.
“Implementing these technologies in a modular plug-and-play approach will allow for adaptability to growing loads over time,” maintains Prochner.
Another way to keep facility options open for the future is to design mechanical systems with extra capacity and redundancy. “For example, air handling units are sized for a lower cooling coil face velocity, ductwork is sized at a lower velocity, fans are designed for higher airflows/static conditions, etc.,” explains Pavel Likhonin, associate, healthcare mechanical department manager at Dewberry. “Plants and mechanical rooms are laid out to show future chillers, pumps, etc.”
To help maximize the life of a new healthcare building, facility managers should ensure that it isn’t designed merely to meet today’s minimum code requirements. “While it is impossible to predetermine if future needs will require greater or lesser provisions, it is possible to plan for such needs,” says Dave Huey, president of Dewberry Architects. “Flexible design considerations must include plans for infrastructure improvements that could require increased capacities, redundancy, varying sizes and utility requirement of replacement equipment.”
“The design has to be resilient, flexible and adaptable,” says Hankin. “A hospital is like a healthcare freeway. Loads change in response to building needs.”
Related Topics:















