 Incorporating cable management for surgical robotics improves infection control while minimizing the disinfection process at the William P. Clements Jr. University Hospital at UT Southwestern Medical Center in Dallas, Tex. (c) CallisonRTKL
Incorporating cable management for surgical robotics improves infection control while minimizing the disinfection process at the William P. Clements Jr. University Hospital at UT Southwestern Medical Center in Dallas, Tex. (c) CallisonRTKLIn Healthcare Facilities, New Technology Improves Energy Efficiency and Comfort
Technology and new modeling software offer facility managers many opportunities to save energy and help ensure visitors are comfortable.
Healthcare facility managers understand the long-term importance of energy-efficient design. Tariq Amlani, principal, buildings health sector Canada, for Stantec, sees demand for energy efficient equipment and finds that healthcare facility managers are interested in energy recovery opportunities.
It’s important to take advantage of software design tools available today. Software can guide “decisions related to orientation on the site; massing; preferred building opening sizes, numbers, and location; and the use of specific materials that will minimize the consumption of energy,” says Huey. Energy modeling is another important tool for targeting opportunities for improvement and setting realistic expectations.
To take advantage of those tools, facility managers have to make energy efficiency a priority from the start of the project. Amlani points to one project where the healthcare facility’s construction would have required excavation of the native soil, which would need to be replaced with nonnative fill. To achieve the stability necessary for the structure, the client opted for a thermal labyrinth, essentially a concrete tunnel, where air can be preheated or precooled using the ground’s natural thermal stability.
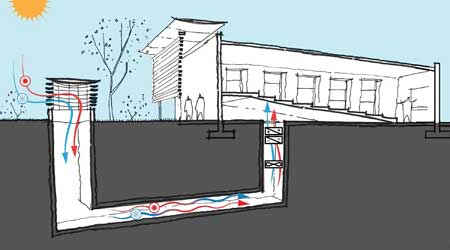

(An underground concrete tunnel known as a thermal labyrinth allows ventilation air to be pre-heated or -cooled using the ground’s thermal stability. Water tanks increase thermal storage capacity. Photo: Stantec)
“This allows them to save on-going operational costs, as well as the capital costs of the nonnative fill,” says Amlani. Solutions like that are possible only if facility managers bring engineering into the design process very early.
Changes in codes could put a new priority on energy performance. “For a long time, healthcare facilities were exempt from building energy codes,” notes Hankin. However, California and Florida now have new energy codes. “This is the first time that healthcare design is being held to the same requirements as other buildings.” Hankin believes this focus on healthcare energy design will be the norm across the United States in the next two to five years.
There are plenty of proven strategies to improve energy efficiency. Likhonin points to installing energy efficient equipment, reducing ductwork runs, reducing internal system losses, and maximizing use of controls and sequences to reduce energy consumption.

(To maximize performance, energy efficiency should be a priority from the very start of a project. For example, energy modeling software can be used to help rightsize a chiller plant. Photo: Ari Burling/Syska Hennessy)
There are also opportunities to control heat gain and loss. Hospitals today are filled with sophisticated medical equipment, much of which generates high levels of heat. If different medical specialties can share space for their advanced equipment — electrophysiology units and interventional radiology in the same space, for example — one air conditioner can supply that room. “That is far more efficient than increasing the size of the hospital’s chiller plant,” Juett explains. “Power, heat exchange, and space requirements are minimized with two separate systems.”
During the design process, technology simulation modeling can be used to examine different building configurations for heat gain and loss. “We even look at finishes and materials from that energy gain-loss standpoint,” Thomas explains.
In addition to orienting the building and simulating solar gain in real time, modeling simulations are done throughout the design process. When an operating room is expanded, for example, the impact on energy use can be assessed.
Comfort and satisfaction
Changes in technology are having a profound impact on comfort and satisfaction. “When it comes to patient comfort, we’re way past just temperature control,” says Krawetz. Hand-held remote controls with downloaded apps can manage lighting, temperature, and blinds as well as television, music, and even nurse call functions. Those technologies can improve ergonomics if the controls can be installed in a way that no longer requires the patient to reach over the bed’s safety rails to a bedside stand, Juett says.
Tunable LEDs make it possible to provide lighting to match human circadian rhythms, by altering the wavelength of the light to replicate the time of day, he says. And lighting can be tuned so that both patient and staff needs are met.
“The healthcare design process requires understanding patient needs and mapping those needs from the minute they come to the facility until the minute they are discharged,” explains Thomas.
It’s important to consider the technological aides nurses and doctors are using in administering patient care. Mobile phones and wireless laptops need charging. “Convenience power can then be installed in waiting spaces and near work areas, allowing them to plug in small devices as they are making rounds, rather than run back to their offices,” explains Juett. Standup stations for doctors can allow them to quickly catch a bit more power for their laptops while handing off nursing instructions.
Related Topics:

















